MobleyMD is recognized internationally as one of the top Facial Plastic Surgery practices in the US.






EXTRACORPOREAL SEPTOPLASTY
Going above & beyond.
Have you been told your nose is too complex to repair surgically? Maybe you have already had one or two surgeries on your nose and a specialist has told you nothing more can be done. Dr. Mobley is known nationally for taking on some of the most complex noses that surgeons see. Dr. Mobley can many times achieve a remarkable result even when other specialists have told you that you can not be helped with surgery.
Dr. Mobley has published two landmark articles describing his pioneering methods of the advanced septal straightening surgical technique called Extracorporeal Septoplasty.
To learn more and to read these landmark articles, click on the thumbnails to download the corresponding PDFs.
FUNCTIONAL SURGERY
Deviated Nasal Septums
The nasal septum is made up of cartilage (in the front) and bone (posteriorly) and is the ”middle wall” inside the nose that divides the left and right nasal passages. Ideally, it should sit in the middle of the nose so that there is an equal-sized air passage on both sides. However, trauma or anatomical deformities can cause the septum to deviate off of the midline, often resulting in nasal obstruction on the side of the deviation.

SEE WHY PATIENTS FLY FROM ALL OVER THE US TO EXPERIENCE DR. MOBLEY AND HIS TEAM’S EXPERTISE IN FACIAL PLASTIC SURGERY.
Dr. Mobley is proud to lead the way in establishing Utah as a major destination hub for Facial Plastic Surgery. Whether you’re from out of state or out of country, our Patient Care Team is dedicated to making your experience with us as simple, efficient and discreet as possible.
What is a Deviated Nasal Septum?
Studies have shown that up to 75% of the general population has some type of deviated nasal septum so simply having a deviated septum does not mean that you need surgery. However, a fair number of people with a deviated septum also develop symptoms that begin to worsen nasal breathing and eventually comprise the quality of life we get from a well functioning nose. The most common symptom of deviated septum is having one side of your nose always more restricted to airflow vs. the “normal” side. Some septums zigzag side-to-side thus restricting airflow through both sides of the nose.Other common deviated septum symptoms include: chronic nosebleeds, sinus infections, congestion, blocked breathing, trouble breathing at night and snoring.
Not sure exactly what type of functional nasal surgery is right for you? Please use Dr. Mobley’s proprietary “Nasal Symptom Checker” to find out if functional nasal surgery from Dr. Mobley may improve your quality of life.
Deviated Septum Diagnosis
Each patient at Mobley Md will undergo a thorough history and physical focusing on factors that affect nasal breathing. A combination of 3 modalities are used to accurately diagnose each patient’s cause of restricted nasal airflow. A simple anterior (speculum) examination will often detect septal deviations, especially those that are located more anteriorly. A nasal endoscopy is performed by sliding a tiny camera mounted on a slender telescope and passing it through the nostrils. This procedure is well tolerated, and although some patients may prefer a numbing nasal spray prior to the procedure, generally an endoscopy can be completed with no special medications at all. This procedure is necessary in approximately a third of patients during their initial consultation.In cases of more complex septal deviations, a CT scan may be necessary. The CT scanner will create a high quality image of the nose, sinuses and surrounding structures and provides the most complete radiological evaluation of nasal function.
Medical Treatment of Deviated Nasal Septum
Septoplasty, or nasal- septal reconstruction, is a procedure meant to straighten the deviated cartilage and bone that make up the nasal septum. In short, the mucosal lining covering the septum is temporarily lifted off of the cartilage and bone. The areas of deviation are usually removed and then replaced back in the midline of the nose. While each case is unique Dr. Mobley tends to avoid techniques that involve a technique called “scoring”. Some surgeons will say they simply ‘score’ the septal cartilage and thereby weaken it, instead of actually removing the deviated segment.
Scoring the cartilage means that the surgeon makes partial cuts into the cartilage with the goal straightening the septum. Unfortunately, cartilage has what is called ‘memory’ – meaning it wants to go back to its original shape if left intact. In some cases where scoring is performed’ over time the cartilage will often times simply bend back to its crooked position once the healing process takes place. This is why some patients (and surgeons) mistakenly say their septum ‘grew back’ after a prior septoplasty. In fact, what happened is that the septal memory caused the nasal septum to return to original and deviated position. This is a common cause of needing a revision septoplasty- a procedure where Dr. Mobley has particular expertise.Septoplasty is performed as an outpatient procedure and usually takes under one hour. Certain patients, such as those with symptoms of sleep apnea or older patients may be encouraged to spend an overnight stay in the hospital just for extra close postoperative monitoring.
Steven Mobley, MD has gained national and international recognition for taking on some of the most complicated cases of nasal septum reconstruction. This type of operation, referred to as “Extracorporeal Septoplasty” is a technique initially developed in Germany but Dr. Mobley performs it routinely for many of the challenging cases sent to him by other ENTs around Utah and around the nation. You can learn more about the specifics of Dr. Mobley’s Extracorporeal Technique for those that want a more detailed explanation of the procedure.
Deviated Septum Surgery
Medical treatments will never actually straighten a nasal septum but for some patients can provide symptomatic relief. There are many medications available and some time just some trials of different medications will be necessary to determine if medical therapy is right for you. Medications can be used to ease symptoms. Some options include: Decongestants (Sudafed, Mucinex-D), Antihistamines (Allegra, Claritin, Clarinex, Zyrtec, Xyzal), Nasal steroids (Nasonex, Nasacort, Veramyst, Omnaris, Flonase), nasal antihistamines (Astepro, Patanase).
If allergies are exacerbating the deviation, then patients may benefit from allergy treatment. Treating allergies will decrease the swelling of the lining of the nasal septum and surrounding tissue. Patients will notice less congestion, but it is important to keep in mind that this will not alter or fix the septal deviation.Medical treatments can be affective in approximately half of patients. However, many of these medications must be taken more or less for life. And a common side effect of these medications is nasal drying which can lead to other problems such as a dry irritated nose and recurring nose bleeds. Utah is one of the driest states in the nation and as such many patients find the daily use of medications just not a practical long-term solution.
Recovery Time After Nasal Surgery
Recovery time can vary based on how much septal reconstruction is performed. For patients with more office type occupations or “telecommuters”, patients can be back at work in as little as 2-3 days. For patients with more physically demanding jobs a period of 7-10 days of recuperation can be more appropriate. One of the many reasons Dr. Mobley continues to get such excellent results is that he follows his patients very closely post operatively. There is flexibility to when you schedule these post op visits, but patients are normally seen the day after surgery, one week after surgery and then a final visit 2 months after surgery. For our many patients from out of town, we can customize the post op visits to fit your overall ability to return to the office.
RELATED PROCEDURES
Other related procedures may include the following:
Before & After Photos
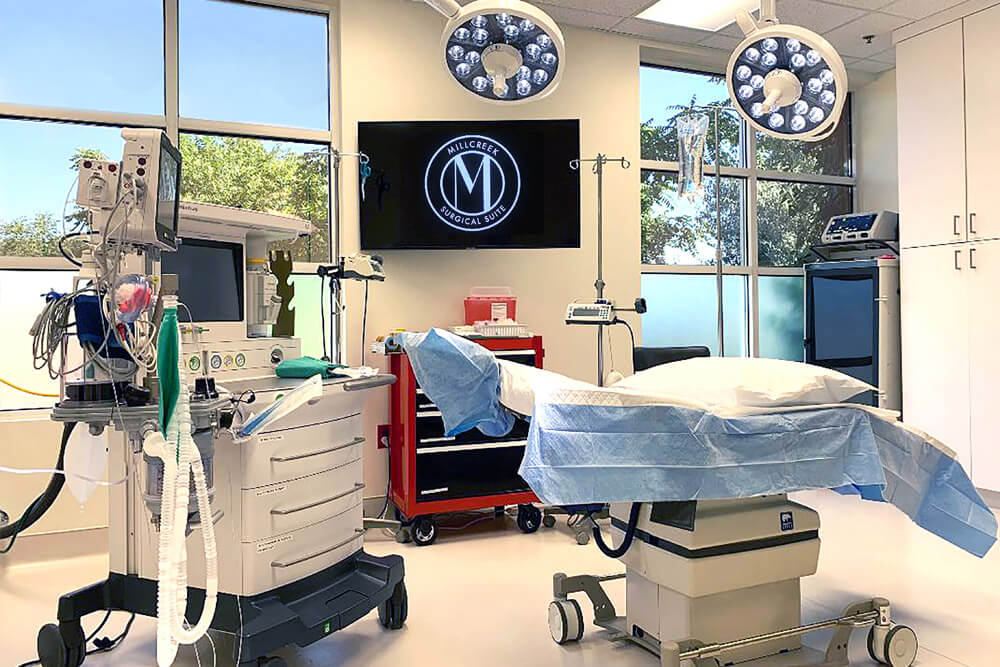
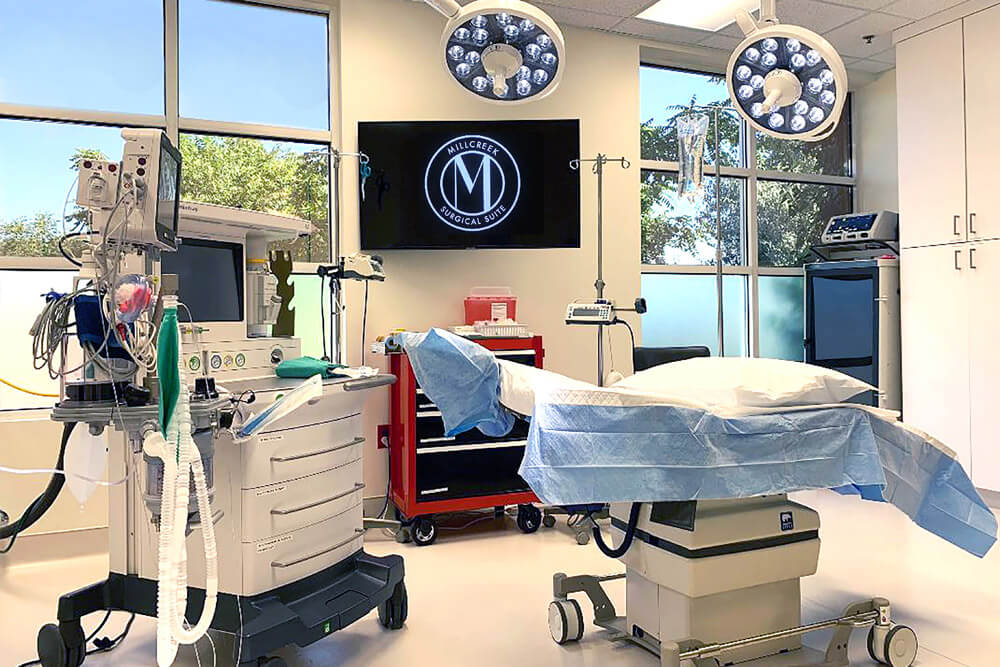
AN OFFICE INSPIRED BY INNOVATION
Experience our state of the art facility in the heart of Utah's Medical Corridor!
Mobley MD Facial Plastic Surgery office was built from the ground up and designed specifically for the patient experience. Our patients have exclusive access to Millcreek Surgical Suite, a AAASF nationally certified center that provides an unparalleled experience for discerning cosmetic patients. Located steps away from Utah’s renowned St. Marks Hospital, our office houses our state of the art surgical facility and our boutique medical spa, BeautyNow.